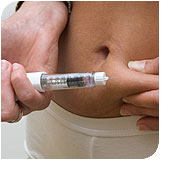
 When patients are diagnosed with multiple sclerosis, then they are usually placed on immunomodulating therapy. The goal of this therapy is to prevent future attacks and future disability.In the United States, there are five immunomodulating drugs approved for the prevention of future attacks in MS. Three of them belong to a class of medications called beta-interferons, one is a different type of protein called Glatiramer acetate, and the fifth drug belongs to a class of medication called SAM blockers. The trade names of the five drugs are Avonex®, Betaseron®, Copaxone®, and Rebif® and Tysabri®.
When patients are diagnosed with multiple sclerosis, then they are usually placed on immunomodulating therapy. The goal of this therapy is to prevent future attacks and future disability.In the United States, there are five immunomodulating drugs approved for the prevention of future attacks in MS. Three of them belong to a class of medications called beta-interferons, one is a different type of protein called Glatiramer acetate, and the fifth drug belongs to a class of medication called SAM blockers. The trade names of the five drugs are Avonex®, Betaseron®, Copaxone®, and Rebif® and Tysabri®.
Copaxone® is glatiramer acetate and is quite different from the other medications. There has been one head to head trial between Copaxone® and Rebif®. This trial demonstrated them to be roughly equivalence. There has been one head to head trial between Copaxone® and Betaseron®. Copaxone® can cause skin lesions and is occasionally associated with chest pain. No blood monitoring is required. Copaxone® requires daily injections.
The three interferons, Avonex®, Betaseron, and Rebif® vary between each other in the route and/or frequency of administration and total dose. One head to head study between Avonex® and Rebif ®has demonstrated that Rebif® prevents more relapses than Avonex®. A second head to head study between Betaseron® and Avonex® demonstrated Betaseron® to prevent more attacks than Avonex®. Avonex® is only given once weekly and some patients find this desirable. Betaseron® is given every other day. Rebif® is given every Monday, Wednesday, and Friday.
This fifth drug, Tysabri®, is a monthly infusion in the physicians office or similar location. Tysabri is the newest therapy available and has its own page on this web site. All five have been shown to reduce the incidence of recurrent attacks in relapsing-remitting MS. There is strong evidence to show the number of MS attacks continue to decrease the longer that any of these medications are taken. There is some data to show that disability decreases as well but this data is less proven (it would be extremely difficult to perform the long-term placebo controlled studies needed to answer this question.
The interferons as a group are sometimes associated with antibody formation, which may limit the effectiveness of the medication, but even this is somewhat controversial. When a patient has side effects and is unable to take one of the medications, then they should be switched to another medication, which is not likely to produce the same side effect. There is also no clear data to guide physicians as to when to switch from one medication to another for patients who are continuing to have MS attacks. Patients and their physicians need to communicate with one another to determine together when to start immunotherapy and to decide which medication to begin. The decision to switch therapy is also very subjective and again it is important for physicians and their patients to communicate.Once immunotherapy is started, it is generally continued for life in patients who respond to the medication.
The only recommended exception in this case is the desire of a patient to become pregnant. In this case, patients should stop the immunomodulating therapy prior to attempting to become pregnant. The effect on the patient's long-term disability by stopping the immunomodulating drugs in order to become pregnant is not known.
For patients who continue to have frequent disabling attacks despite immunomodulating therapy or for those who begin to accumulate deficits, then stronger immunosuppressive treatment is commonly recommended. Recently, Novantrone® or mitoxantrone has been approved for the treatment of this group of patients. Other medications and treatments that are considered after mitoxantrone include medications such as cyclophosphamide, cyclosporin, IVIG, and procedures such as a bone marrow transplant.



