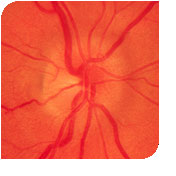
 The optic nerve is a relatively small part of the central nervous system that carries information from the retina of the eye to the optic chiasm. In the chiasm, the fibers from the left side of the visual field from each eye pair up and proceed to the thalmus in the optic tract. In front of the chiasm, the optic nerve carries information from only one eye. For reasons that are not explained, multiple sclerosis disproportionately favors attacking the optic nerve. When this occurs, one has optic neuritis. Optic neuritis can be silent or sufficient to cause blindness, it can be painful or painless.
The optic nerve is a relatively small part of the central nervous system that carries information from the retina of the eye to the optic chiasm. In the chiasm, the fibers from the left side of the visual field from each eye pair up and proceed to the thalmus in the optic tract. In front of the chiasm, the optic nerve carries information from only one eye. For reasons that are not explained, multiple sclerosis disproportionately favors attacking the optic nerve. When this occurs, one has optic neuritis. Optic neuritis can be silent or sufficient to cause blindness, it can be painful or painless.
It had been known for many years that treating patients with optic neuritis would make their vision return faster. Not until the optic neuritis treatment trial, when patients were randomly assigned to IV steroids (Solumedrol or methylprednisolone) followed by oral steroids (prednisone), oral steroids alone, or no treatment was it clearly determined that ultimately, being treated with steroids during the acute phase did not apparently affect the long term vision outcome.
In this study, those treated with only the oral steroids, seem to relapse at a higher rate than the IV steroid group or the placebo group. For this reason, the use of IV steroids or no treatment, has become routine care for patients who present with optic neuritis without a history of multiple sclerosis.Fortunately, the patients in this study were followed for many years and there is some information available as to the future of patients who have an attack of optic neuritis. For those who have an MRI with 3 or more lesions felt to be compatible with multiple sclerosis, then at five years about half of the patients definitely had multiple sclerosis. At ten years, the chance of having multiple sclerosis was about 60%.
For those who had an abnormal MRI with only 1 lesions, they developed MS at a slower rate with about one third having MS in 5 years but about 50% having MS at 10 years. For those patients with a normal MRI and CSF findings that did show oligoclonal bands, the five year chance of developing multiple sclerosis was about one in four. Among the twenty-eight patients who had a normal MRI and no finding of oligoclonal bands in their CSF, only one, or four percent, developed multiple sclerosis by five years. I have not seen published data for the 10 year follow up of those patients who had CSF taken. The overall 10 year risk of having MS with a normal MRI is 20% but again a breakdown on patients with and without oligoclonal bands on MRI are not given.
For those who would like to review the original articles, the five year data was published in the Journal Neurology, (Neurology, 1997; 49:1404-1413) and the 10 year data in the Journal Archives of Opthamology, (Arch Ophthalmol. 2003 Jul;121(7):949-9).From the information above, many physicians who treat patients with multiple sclerosis will place patients who have a history of optic neuritis and an abnormal MRI with three of more lesions on immunomodulating drugs.



